During pregnancy, water is vital to your health and your baby’s health. Pregnancy is associated and leads to a significant weight gain, which averages 12 kg (26lb) at term in women with a healthy BMI (IoM, 2009).
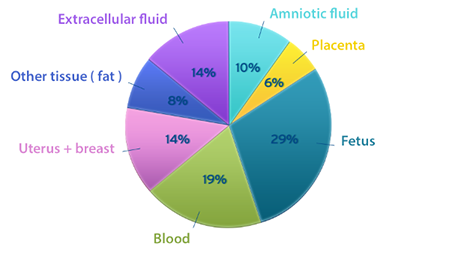
The major contributor to this weight gain is water. It increases 1.5 to 2 gallons in healthy pregnant women during pregnancy. (2)
Where does all this water go? Water helps to form your placenta, build your amniotic fluid and increase blood volume for the benefit of your little one. Your baby is mostly water about 80% (2), and all of that water has to come from you.
So it is essential you stay hydrated during pregnancy. You need to take care of yourself (including your health and diet) to ensure the best start in life for your precious bundle of joy.
If you aren’t drinking enough water, dehydration can occur. Dehydration describes when your body doesn’t have enough water and other fluids to function properly. Dehydration can range from mild to severe, but even mild dehydration can be dangerous for pregnant women.
Mild dehydration can cause low energy levels and depressed moods. That’s the last thing a pregnant momma needs! Dehydration can lead to more serious problems, such as a low amniotic fluid.
Amniotic Fluid
Amniotic fluid is the fluid that surrounds your baby within the amniotic sac (amnion). Amniotic fluid serves as a shock absorber and protects your unborn child from physical harm. It also protects your baby from infection. Amniotic fluid helps your baby’s lungs and digestive system to grow and mature properly.
In a healthy pregnancy, the amount of amniotic fluid increases each week, until a few weeks before full-term. At the peak, the average pregnant woman carries about 27 ounces of amniotic fluid. After reaching its peak, the amount of amniotic fluid gradually decreases until the baby is born.
When you’re pregnant, your doctor will monitor your amniotic fluid levels to ensure they’re within proper ranges. Complications increase if there is too much, or too little, amniotic fluid.
Ultrasound is the best tool for evaluating amniotic fluid levels
Ultrasound is the only practical tool for assessing amniotic fluid level while pregnant. A regular Black/white (or 2-D) ultrasound measure amniotic fluid levels by obtaining either an amniotic fluid index (AFI) measurement or a single deepest pocket (SDP) measurement. Your doctor should review these measurements each time you receive an ultrasound that has included gauging the fluid levels.
Ultrasound is the best method for your doctor to ensure you have enough, but not too much, amniotic fluid.
Too Little Amniotic Fluid (Oligohydramnios)
Your doctor may be concerned if there is not enough amniotic fluid if your SDP is less than 2 cm, or your AFI is less than 5 cm. Not having enough amniotic fluid is called oligohydramnios. Oligohydramnios can be caused by a variety of reasons, including dehydration (3). Not enough amniotic fluid early in the pregnancy can lead to congenital abnormalities or miscarriage.
In later stages of pregnancy, oligohydramnios can cause labor complications and pre-term birth. During the second and third trimester, there are only three reasons for contractions: full-term birth, bladder infection or pre-term labor. If you’re severely dehydrated, your blood volume decreases, which can raise the concentration of oxytocin. Since oxytocin induces contractions, it can lead to premature labor.
Too Much Amniotic Fluid (Polyhydramnios)
Your physician will get concerned if your baby has too much amniotic fluid around it if your largest fluid pocket depth (maximal vertical pocket (MVP) greater than 8 cm, or your overall AFI (Amniotic Fluid Volume) exceeds 25 cm.
Having too much amniotic fluid surrounding your baby is called polyhydramnios. It is a relatively rare condition only occurring in about 1% to 3% of pregnancies. There are many reasons you may have too much amniotic fluid. Maternal causes, multiple births, and even unknown reasons can result in polyhydramnios.
Most women with polyhydramnios give birth to healthy babies, so don’t worry yet. Familiarize yourself with possible effects of polyhydramnios, such as early or premature labor. In some polyhydramnios cases, the baby does not turn before birth, requiring a cesarean section for delivery.
Talk to your doctor about risks and options if they’re concerned about your amniotic fluid levels.
Healthy Hydration for Best 3D Ultrasound Pictures
While elective 3-D ultrasounds are not practical for measuring amniotic fluid levels or determining if you’re dehydrated, they are still a very fun and important part of pregnancy! If you’re having a 3-D ultrasound performed, be sure to stay well hydrated before your scan. Good hydration is not only good for you and your baby; it helps to get the best 3D Ultrasound pictures!
We advise that you check with your OB provider on the amount of daily fluid intake and starting to drink the amount of the fluid recommended by your doctor at least a week before your 4D ultrasound scan will lead to the best ultrasound results.
The sound waves of a 3D/4D ultrasound pass through fluid easily and a pocket of the fluid around the baby’s face is required to obtain a good 3D ultrasound picture that will highlight facial features in great details, so this is why more fluid produces better quality ultrasound pictures.
It takes about two to four days for water you drink to affect the fluid levels in your uterus. That’s why it’s important to plan your fluid intake for an entire week before your scheduled ultrasound procedure. Last minute increases in water intake do not affect your uterus quickly enough.
Please note, drinking enough fluid for your elective ultrasound does not mean you will need a full bladder for an excellent 3D/4D ultrasound picture. You do not (thankfully) have to hold off on relieving yourself before your 4D scan. Just try to retain your recommended intake of fluids for the week before your 3D sonogram scan. You’ll appreciate it later when you’re looking at those incredible pictures of your little one(s).
Complications & Side Effects of Dehydration during Pregnancy
Dehydration can cause other complications to both mother and child. Although not common, dehydration can cause spotting in pregnancy. It’s believed some women experience spotting when dehydrated, as their hCG levels temporarily stop increasing, or dip.
Once re-hydration is reached, hCG levels level out and spotting may stop. Sometimes, bleeding during pregnancy may be a sign of a threatened miscarriage. Moderate or severe dehydration may cause a threatened miscarriage.
Severe dehydration during pregnancy can induce serious complications such as blood clots, neural tube defects, and seizures. Dehydration while pregnant can increase body temperature, which can complicate heat-related issues such as muscle cramping and heat exhaustion. Continued dehydration can lead to inadequate breast milk production and changes in breast milk composition.
Preventing Dehydration
Because of the risks of dehydration, while pregnant, it’s important you stay as hydrated as possible by following your doctors’ advice. While pregnant, your total water intake (from food and drinks) should be about 100 ounces per day.
Your fluid intake (from just-drinks) should be a minimum of approximately 64 ounces, or 8 cups, per day. Please, check with your OB provider to make sure the amounts provided are matching your particular situation.
Remember, everything you drink, including water, coffee, tea, juice, milk and even caffeinated sodas count toward your total fluid intake. Although it’s healthiest to drink primarily water, it’s almost impossible in real life, especially when you’re pregnant. Occasional caffeine won’t be a problem, but it might increase your urine output as it is considered a diuretic. In other words, it might make you pee more!
Every pregnant woman understands morning sickness can make it difficult to intake enough fluid! Not only are you feeling tired and sick – you may be vomiting without warning. Vomiting, of course, increases your chances of dehydration.
Some tips to help nausea and stay hydrated, especially when you’re pregnant:
• If you have nausea mostly in the morning, start your day with something other than plain water. Just as crackers can help settle a stomach, flavored water, juice or tea can stay down better than plain water on an empty stomach.
• If you don’t find plain water tasty, flavor it with some lemon or another flavor to make it more palatable.
• Try to avoid drinking too much caffeine, as it can decrease hydration by increasing urine output.
• If you’re nauseous and vomiting throughout the day, try drinking some broth (chicken, beef or vegetable). For some women with severe morning sickness, the extra protein, vitamins, and minerals help stay down better than sweet juices or sports drinks.
• Try to keep a bottle within reach at all times and take small sips throughout the day. This will keep your hydration levels more level throughout the day.
• Drink plenty of water before, during and after activity, especially in hot weather.
• Popsicles (which are mostly water) are another great option for hydrating when you don’t want yet another glass of water.
• It’s easier to keep down little bits of drink and food when suffering from morning sickness. Often eating six small, light meals can help women suffering from morning sickness feel better.
• If it’s hot out, drink extra water or fluids to offset the water you’ll lose through sweat.
• Try not to spend too much time in a hot environment. The longer you spend, the more energy your body expends to keep you cool, and the more fluid loss you’ll suffer.
• If it’s hot out, avoid strenuous exercise during the hottest parts of the day. Plan physical activity for early morning or late evening to stay cooler.
• Avoid alcohol, including wine and beer, as alcohol can contribute to dehydration.
Remember, fruits and vegetables are also an excellent source of water. Some fruits and vegetables are mostly water, such as celery and watermelon. Other high-water content fruits and vegetables include strawberries, cantaloupe, cucumber, leafy greens, zucchini, tomatoes and bell peppers. See, it is just like mom said: “Eat your fruits and veggies!”
Electrolytes are chemicals that help your body produce ions in your bodily fluids. These ions carry the energy your body needs to produce movement or work. Many bodily functions rely on electrolytes, such as muscle contractions and nerve impulses.
The proper ratio of electrolytes is critical, as both too much and too little electrolytes can cause problems such as muscle cramping. Your body needs a consistent influx of electrolytes to stay balanced and healthy.
While drinking water is the best thing to stay hydrated, some people prefer sports drinks with electrolytes, or hydration tablets added to water. While sports drinks will replace some of the electrolytes you’ve lost during intense exercise or perspiration, they tend to be high in extra sugar and calories. Water, or flavored water, remains the healthiest choice for staying well hydrated.
Dehydration Treatment
If you think you are mildly dehydrated, you may be able to treat yourself by increasing your fluid intake, but you should talk to your doctor. If you are pregnant and think you are more than mildly dehydrated, please seek immediate medical care. If you think you are severely dehydrated, get immediate medical attention or if life-threatening, call 911.
Signs and symptoms of mild to moderate dehydration include:
• dry skin, mucous membranes
• headache
• sweating too much, or not sweating at all
• few tears when crying
• dizziness or lightheadedness
• constipation (although this can occur without dehydration in pregnant women)
• nausea (although this can also be caused by morning sickness when pregnant)
• dark urine color or strong smelling urine
• minimal urine production
• may feel thirsty; dry or sticky mouth
• muscle cramps
Signs & Symptoms of Moderate and Severe Dehydration:
• lack of urination
• urine that is very dark
• severe thirst
• shriveled skin
• sunken eyes
• severe headache
• low blood pressure
• rapid heartbeat
• rapid breathing
• no tears when crying
• little to no sweat production
• fever
• unconsciousness
• dizziness
• confusion or delirium
1. Givens and Macy, 1933; Ziegler et al. 1976
2. Chesley, 1978; Hytten, 1980
3. Patrielli et al. 2012